Knee pain is one of the most common complaints among adults and active individuals. Whether it stems from arthritis, sports injuries, or natural wear and tear, knee discomfort can limit mobility, impact daily activities, and lower quality of life. Traditionally, many have turned to surgery for relief. However, surgery isn’t always the best—or only—option.
Today, a growing number of people are exploring stem cells for knee repair as a natural, non-invasive solution.
Table of Contents
Why Traditional Knee Surgery Isn’t Always the Best Option
What Is Stem Cell Therapy for Knee Repair?
8 Conditions Treated with Stem Cell Therapy for Knees
9 Benefits of Choosing Stem Cell Therapy Over Surgery
4. Pain Relief and Improved Function
6. Personalized Treatment Approach
7. Lower Overall Cost (in Many Cases)
8. Compatible with Other Therapies
What to Expect Before, During, and After Treatment
How to Choose the Right Provider for Your Knee Stem Cell Therapy
Take the First Step Toward Pain-Free Knees—Choose BioRestore!
| Key Takeaways
✔ Stem cell therapy for knees avoids surgical risks by eliminating the need for general anesthesia, incisions, and reducing the chance of infection, blood clots, or nerve damage. ✔ Recovery is significantly faster with stem cells for knee repair, allowing patients to return to normal activities in days instead of enduring months of post-surgical rehab. ✔ The treatment harnesses natural healing by using the body’s regenerative cells to repair cartilage, tendons, and ligaments. ✔ Stem cell therapy effectively reduces chronic pain by targeting inflammation at the source, resulting in sustained relief and improved joint mobility. ✔ Stem cell therapy can delay or eliminate the need for surgery, especially for patients in the early to moderate stages of joint damage. ✔ Each procedure is personalized and targeted, with stem cells drawn from the patient’s body and injected directly into the damaged knee area. ✔ This approach treats multiple knee conditions, including osteoarthritis, meniscus tears, ligament injuries, and tendonitis without invasive methods. ✔ Stem cell therapy integrates with other therapies like physical rehabilitation and PRP, and it’s safe to repeat for continued benefit. ✔ Patients experience an improved quality of life through enhanced mobility, reduced reliance on pain medications, and restored joint function. |
Why Traditional Knee Surgery Isn’t Always the Best Option
Surgical procedures like arthroscopy, ligament reconstruction, and total or partial knee replacement are often prescribed for chronic or severe knee problems. However, they are not without risks—and not always necessary for every case. For many, especially those in the early or moderate stages of joint deterioration, stem cell therapy for knees offers a safer and more natural alternative.
While knee surgery has its place for certain severe cases, many patients can benefit from less invasive, regenerative options. For those wondering, “how effective is stem cell therapy for knees” or “does stem cell therapy for knees work”, the potential to heal naturally, avoid surgery, and restore function makes it a compelling alternative worth exploring.
1. Risks of General Anesthesia
- Unpredictable reactions: Some patients experience adverse effects such as breathing problems or allergic responses.
- Age and health-related complications: Older adults and those with preexisting conditions face higher anesthesia-related risks.
2. Post-Surgical Complications
- Infection risk: Any open surgery creates a pathway for bacteria, increasing the risk of joint or wound infections.
- Blood clots and DVT: Limited movement during recovery may lead to clot formation in the legs, which can be life-threatening if not addressed.
- Nerve or tissue damage: Even skilled surgeons can’t fully eliminate the risk of unintended injury during surgery.
3. Long and Challenging Recovery
- Extended downtime: Recovery can span several months, often requiring time off work and help with daily tasks.
- Physical therapy required: Rehabilitation is intensive and often painful, with no guarantees of full mobility restoration.
- Delayed return to activity: For athletes and active individuals, being sidelined for months can be both frustrating and debilitating.
4. Irreversible Procedures
- Permanent changes to the joint: Once bone or cartilage is removed or replaced, it cannot be restored to its original state.
- Artificial joint limitations: Prosthetic implants may not feel or function like natural joints and often have a lifespan, leading to potential revision surgeries later.
5. Not Always Successful
- Uncertain outcomes: Some patients continue to experience pain, stiffness, or instability even after technically “successful” surgery.
- Scar tissue formation: Excessive scar tissue can limit range of motion and contribute to long-term discomfort.
6. High Financial and Emotional Cost
- Costly medical bills: Hospital stays, anesthesia, physical therapy, and time off work can make surgery financially burdensome.
- Emotional toll: Anxiety about the surgery, extended recovery, and fear of complications often weigh heavily on patients.
7. Not Ideal for Early-Stage Damage
- Overtreatment concerns: Patients with mild to moderate joint issues may not need such an aggressive intervention.
- Opportunity for alternatives: Stem cell for knee repair provides a proactive option that targets healing without permanent joint alterations.
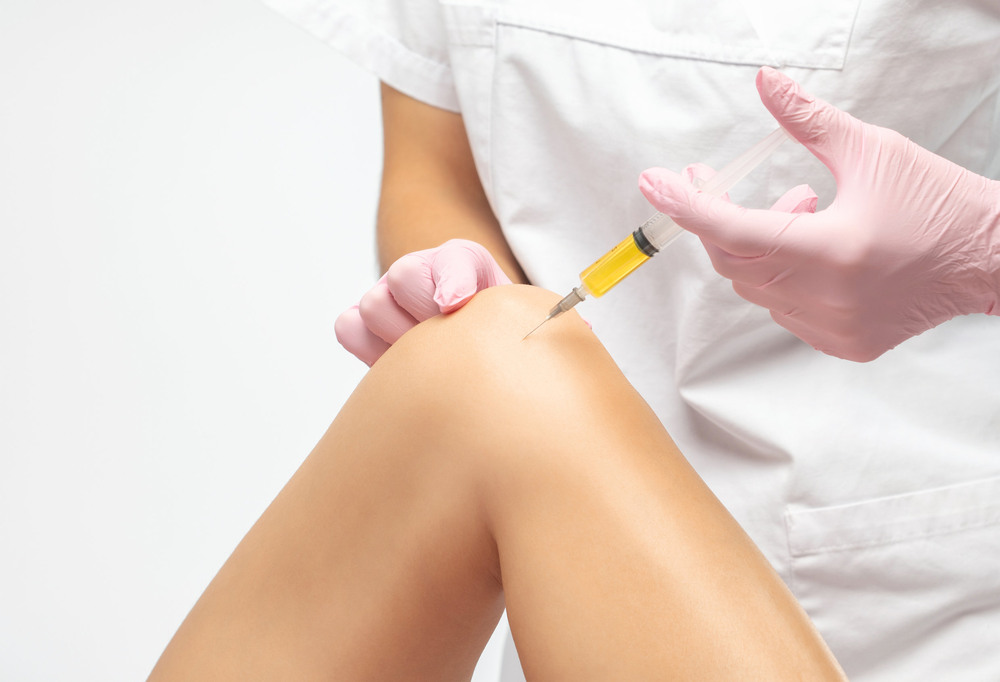
What Is Stem Cell Therapy for Knee Repair?
Stem cell for knee repair involves using the body’s regenerative cells to help repair damaged or inflamed knee tissue. Stem cells are unique because they can develop into different types of cells, including cartilage, bone, and connective tissue. This makes them an ideal candidate for tissue regeneration therapies.
Stem cells are typically harvested from a patient’s bone marrow or fat tissue. These cells are then processed and injected directly into the affected knee joint. Once in the knee, the stem cells go to work by reducing inflammation, stimulating the healing of damaged tissues, and promoting the growth of new, healthy cells.
A systematic review in the Journal of Experimental Orthopaedics analyzed 12 studies involving 539 patients with early to moderate knee osteoarthritis. The review reported that a single intra-articular injection of mesenchymal stem cells led to improvements in patient-reported outcomes, knee function, pain relief, and quality of life.
8 Conditions Treated with Stem Cell Therapy for Knees
For those asking, “does stem cell therapy for knees work?” the range of treatable conditions and the regenerative potential of stem cells make the answer increasingly clear: yes, especially when guided by skilled professionals and early intervention.
By targeting the underlying source of joint damage, stem cell therapy for knees encourages healing and helps patients avoid surgical interventions.
1. Osteoarthritis of the Knee
Osteoarthritis leads to the gradual breakdown of cartilage, reducing the cushion between bones and causing pain, stiffness, and swelling. Stem cells for knees help regenerate cartilage, reduce inflammation, and slow the progression of joint damage. Patients in earlier stages of osteoarthritis often respond best to regenerative treatments.
2. Meniscus Tears
The meniscus is a shock-absorbing disc in the knee that can tear due to twisting, squatting, or aging. Meniscectomy (removal of part of the meniscus) can speed up joint deterioration. Stem cell for knee repair works to restore the integrity of the meniscus rather than removing it, preserving long-term joint health.
3. Ligament Injuries (ACL, MCL)
Sudden stops, twists, or impacts can damage major ligaments like the anterior cruciate ligament (ACL) and medial collateral ligament (MCL). Traditional repairs often involve grafts and long recovery times. Stem cells for knees promote the healing of partially torn ligaments and strengthen weakened areas without invasive procedures.
4. Patellar Tendonitis and Other Tendon Injuries
Activities involving jumping, running, or repetitive stress can inflame or damage knee tendons. Tendonitis often lingers and may become resistant to conventional therapies like anti-inflammatories or corticosteroids. Stem cell therapy for knees can reduce inflammation and stimulate tendon repair at a cellular level.
5. Chondromalacia Patella (Runner’s Knee)
Cartilage softening behind the kneecap causes grinding pain during movement, especially stairs or squats. This typically affects young adults and athletes, especially those involved in high-impact sports. Stem cell therapy helps regenerate cartilage and soothe inflamed tissue without invasive correction.
6. Post-Traumatic Knee Injuries
Even after initial healing, past trauma can result in chronic instability or pain. Physical therapy and medication often fall short in restoring full function. Stem cell for knee repair assists in healing old damage, restoring strength and mobility to compromised areas.
7. Cartilage Defects or Lesions
Focal cartilage injuries can result from impact, joint misalignment, or repetitive stress. If left untreated, lesions can develop into widespread arthritis. Promotes cartilage regeneration and helps fill in defects without surgical grafts or implants.
8. Bursitis
Bursae are fluid-filled sacs that cushion the joint; inflammation can lead to pain and swelling. This is often caused by pressure or overuse, and is especially common in those who kneel frequently. Stem cell therapy reduces inflammation and promotes tissue balance, offering lasting relief.
9 Benefits of Choosing Stem Cell Therapy Over Surgery
There are numerous advantages to choosing stem cell for knee repair, especially when compared to traditional knee surgeries like arthroscopy or total joint replacement. This regenerative approach prioritizes natural healing, patient comfort, and long-term function.
1. Minimally Invasive
- No scalpels or stitches required: The entire procedure involves a simple injection rather than incisions.
- Outpatient convenience: Most sessions are done in-office, avoiding the need for hospital stays or general anesthesia.
- Lower risk of complications: There’s reduced potential for infection, blood clots, and scarring compared to surgery.
2. Shorter Recovery Time
- Faster return to activity: Most individuals resume light activity within days, not months.
- No need for intensive rehab: Physical therapy is often gentler and less prolonged than post-operative rehabilitation.
- Minimal disruption to lifestyle: This makes stem cells for knees ideal for working adults, parents, and active seniors.
3. Natural Healing
- Biological regeneration: The body uses its own cells to repair damage, rather than replacing tissues or joints with artificial materials.
- Supports tissue growth: Stem cells release growth factors that aid in repairing cartilage, tendons, and ligaments.
- No foreign implants: This reduces the risk of rejection, inflammation, or implant failure down the line.
4. Pain Relief and Improved Function
- Anti-inflammatory effects: Stem cells actively reduce inflammation, which is often the root cause of chronic knee pain.
- Gradual but real improvements: Many report sustained relief and improved joint movement within weeks to months.
- Clinical support: Wondering how effective is stem cell therapy for knees? Multiple studies suggest real-world effectiveness in improving range of motion and reducing discomfort.
- Proven outcomes: A clinical trial reported that a single injection of an off-the-shelf stem cell therapy significantly improved pain and function for up to 12 months in 75% of participants with knee osteoarthritis.
5. Delays or Avoids Surgery
- Proactive joint care: Treating knee damage early can prevent worsening conditions that may eventually require surgery.
- Reduced surgical burden: Even if surgery is needed in the future, patients may benefit from improved joint health in the interim.
6. Personalized Treatment Approach
- Custom cell harvesting: Stem cells are drawn from the patient’s own tissue, ensuring a match.
- Tailored injections: The dosage and injection site can be adjusted based on the patient’s condition and imaging results.
- Physician-guided protocols: Providers can incorporate this therapy into broader joint health strategies for comprehensive care.
7. Lower Overall Cost (in Many Cases)
- Avoids hospital fees: No operating room or extended inpatient care needed.
- Less need for post-op medications: Reduced reliance on painkillers and anti-inflammatory drugs.
- Fewer workdays lost: With quicker recovery, many return to work and daily life sooner, minimizing economic impact.
8. Compatible with Other Therapies
- Integrates with physical therapy: Patients can enhance their outcomes through guided exercise and strengthening.
- Safe to repeat if needed: Some patients undergo multiple rounds of stem cell for knee repair to maximize benefits.
- Pairs with PRP: Platelet-rich plasma (PRP) is sometimes combined with stem cells to further stimulate healing.
9. Improved Quality of Life
- Better mobility and flexibility: Daily activities such as walking, climbing stairs, and exercising become more manageable.
- Reduced reliance on medications: Less need for NSAIDs or corticosteroid injections for chronic pain.
- Greater confidence in movement: Reduced pain leads to more independence and overall wellness.

What to Expect Before, During, and After Treatment
Understanding each phase of the stem cell for knee repair process helps patients prepare physically and mentally for the journey. Here’s a clear breakdown of what happens before, during, and after treatment.
Before Treatment: Evaluation and Preparation
- Comprehensive consultation: A licensed provider will review the patient’s medical history, symptoms, and previous treatments to determine suitability for stem cell therapy for the knees.
- Imaging and diagnostics: Tools like X-rays, MRIs, or ultrasounds are used to pinpoint areas of joint damage and inflammation.
- Functional assessment: Range of motion, joint stability, and pain levels are measured to create a personalized treatment plan.
- Medication and supplement guidance: Patients may be advised to pause anti-inflammatory drugs that could interfere with the regenerative process.
- Lifestyle instructions: Pre-treatment guidance may include hydration, light activity, and avoiding smoking to enhance stem cell viability.
During Treatment: The Regenerative Procedure
- Stem cell harvesting:
- Bone marrow draw: Extracted from the pelvic bone under local anesthesia.
- Adipose tissue draw: Obtained from abdominal fat using a minor liposuction-like procedure.
- Bone marrow draw: Extracted from the pelvic bone under local anesthesia.
- Cell processing: The collected tissue is spun in a centrifuge to concentrate the stem cells and separate them from other components.
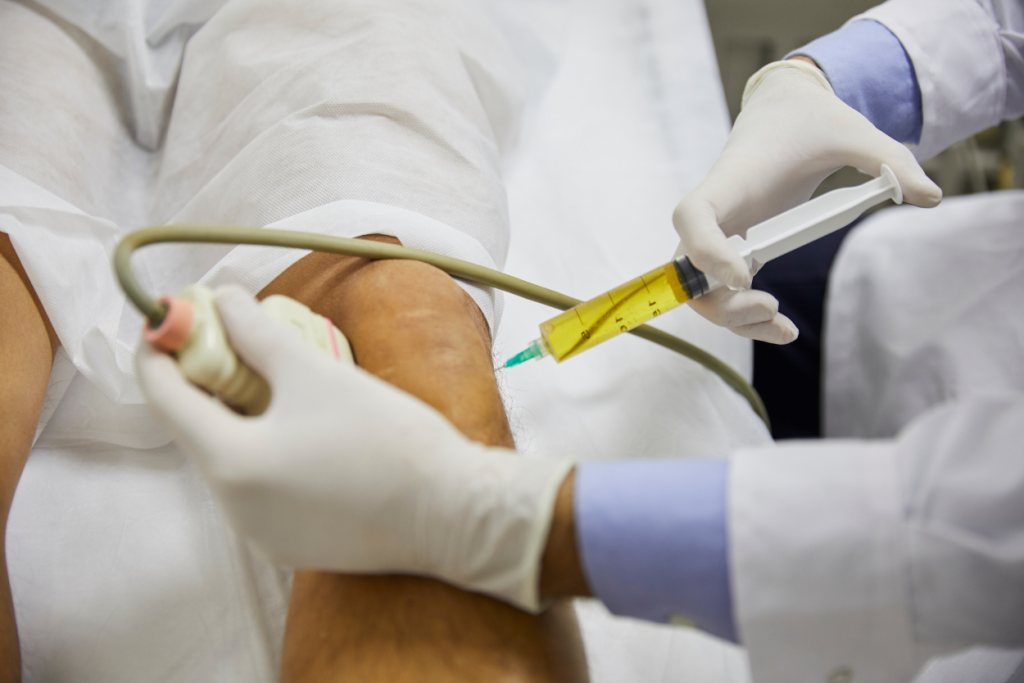
- Injection into the knee joint: The targeted knee is cleaned and numbed with local anesthetic. Using ultrasound or fluoroscopic guidance, the physician injects the prepared stem cells for the knees directly into the damaged area.
- Quick outpatient session: The entire process typically takes 60–90 minutes, and patients can return home the same day.
After Treatment: Recovery and Results
- Immediate post-procedure care: Light rest is recommended for the first 24–48 hours. Ice may be used to manage minor swelling or discomfort at the injection site.
- Gradual return to activity: Patients can resume daily activities within a few days. High-impact or strenuous movements should be avoided until cleared by the provider.
- Customized rehabilitation plan: Physical therapy or stretching exercises may be introduced to support healing and improve joint function. Some protocols include bracing or offloading to protect the joint.
- Monitoring and follow-ups: Progress is evaluated at regular intervals through movement assessments or imaging. Additional injections may be suggested for advanced degeneration or a slower healing response.
- Expected results timeline: Pain relief and functional improvements are typically seen within 2 to 8 weeks. Full benefits may continue to develop over 3 to 6 months as the regenerative process unfolds.

How to Choose the Right Provider for Your Knee Stem Cell Therapy
Selecting the right clinic is essential for successful stem cell for knee repair. Not all providers have the same level of experience or training in regenerative medicine.
1. Look for Expertise
Choose a provider who specializes in stem cell therapy for knees and has a proven track record of success. If you’ve been asking yourself, “does stem cell therapy for knees work?”—experience and results from past patients can be a strong indicator. Board certifications in orthopedics or regenerative medicine can also add credibility.
2. Ask the Right Questions
During the consultation, patients should ask:
- Where are the stem cells harvested from?
- Is the procedure done in-office or at a surgical center?
- How many patients have you treated with stem cells for knees?
- How effective is stem cell therapy for knees in your experience?
3. Consider Safety and Technology
The clinic should use sterile, advanced equipment for cell processing and injection. Imaging guidance (like ultrasound or fluoroscopy) improves the accuracy of injection and overall success of the treatment.
4. Evaluate the Consultation Process
A thorough evaluation before proceeding with treatment shows that the provider is cautious and patient-centered. Clinics that recommend stem cell for knee repair without proper diagnostics should be approached with caution.
Frequently Asked Questions
Yes, many patients report reduced pain, improved mobility, and better joint function after stem cell therapy for knees. The treatment works by reducing inflammation and promoting tissue regeneration. Effectiveness varies by condition severity and individual response.
Studies show success rates ranging from 60% to 85% for patients with mild to moderate knee degeneration. Success is defined by pain relief, increased function, and delayed need for surgery. Outcomes depend on the patient’s health, condition type, and provider expertise.
Most patients experience minimal side effects like temporary swelling, soreness, or bruising at the injection site. Serious complications are rare, especially when using autologous (self-derived) stem cells. However, results may vary, and some patients may not experience full relief.
Ideal candidates include individuals with early to moderate knee osteoarthritis, ligament injuries, or chronic inflammation not responding to other treatments. It’s best for those looking to avoid or delay surgery. A thorough evaluation and imaging will determine eligibility.
Results can last anywhere from 6 months to several years, depending on the condition treated and patient activity levels. Some patients benefit from periodic follow-up treatments. Overall, many experience long-term relief and improved function without surgery.

Take the First Step Toward Pain-Free Knees—Choose BioRestore!
If you’re looking to avoid surgery and restore your knee health naturally, BioRestore in Connecticut offers trusted, science-backed stem cell therapy tailored to your needs. Thousands of Connecticut residents have turned to BioRestore for non-invasive knee repair solutions with real, lasting results. Whether you’re in the early stages of knee degeneration or seeking relief from chronic pain, BioRestore in Connecticut is ready to help you regain mobility and live pain-free.
Schedule your consultation with BioRestore today!